 Fondation Ti Ajoupa – Non-Profit Organization
Fondation Ti Ajoupa – Non-Profit Organization
This case study intends to illustrate issues that health-based organizations face in Haiti. It does not intend to provide a blueprint as to how organization should be run. As with all case studies, it does not provide answers but poses questions that can be tackled by interested parties. This document looks at the management aspects of health organizations rather than an in-depth review of the medical services rendered by a mobile clinic. This case study focuses on the operational and project management aspects of health-based organizations.
D. Alain Menelas
C.Paribus Management
Rethinking Mobile Health Clinics in Haiti
Wasted Resources?
It is 4 o’clock at the Toussaint Louverture international airport in Port-au-Prince and Ms. Djenny Pierre is waiting for the airplane that will take her back to Massachusetts. As always, her plane is late and she can’t help but reflect about this trip to Haiti. Ms. Pierre is the director and founder of Banmsantee, a health organization based in Massachusetts and Haiti. Currently, the operations of Banmsantee mostly take place in Massachusetts however Ms. Pierre travels to Haiti often to organize mobile clinics and supervise the completion of her clinic in Les Cayes, a bustling city in the South department.
Ms. Pierre’s flight back to the United States was supposed to be a joyful one. This is the second mobile clinic her organization led. In December 2020, Banmsantee held a free clinic at a Christian church in Les Cayes. On that occasion, she was able to serve 50 people from 7:30 am to 1:30 pm. For this trip, she had scheduled three days of mobile clinics during the month of May for Mother’s Day. Banmsantee expected to serve at least 50 people a day over two days but barely served 50 over the two days combined (See exhibit 1).
Exhibit 1. Mobile clinics and number of patients served
| Date | Number of days | Location | Number of patients |
| December 24, 2020 | 1 | Christian church | 50 patients |
| May 29-30th,2020 | 2 | Local school | 50 patients |
Sitting at the airport, Ms. Pierre believes that it is unfortunate that in a country were most people lack access to health services, her organization was not able to reach more patients. Looking at the tarmac through the large windows, she reflects on the main reason why attendance was so low; her collaborators failed to spread the word and as a result few people knew that she was having a free clinic. How can she make sure that this does not happen again? She wondered, how could she serve 100 people or more a day during her next clinic. Her flight back to Boston was going to be a long one.
Background
Haiti is a country in the Caribbean where 11 million people live. The country shares the island of Hispaniola with the Dominican Republic. Haiti is the poorest country in the western hemisphere with close to 60% of its population living under the poverty line. In 2019, the GDP per capita of the country was estimated to be about U$ 2,905. In 2018, there were 0.23 physicians for every 1000 individuals[1]. In 2010, a devastating earthquake killed about 250,000 Haitians and put significant pressure on already meager health infrastructures. Despite significant international support, access to basic health services remains a challenge especially in rural areas where such services are quasi non-existent. 23 % of the population have access to primary care of good quality; that includes 5% of the rural population.[2]
Mobile clinics in Haiti
Every month, local and international organizations hold mobile clinics in Haiti. A mobile clinic is usually held at a non-permanent location for one or a few days. Many mobile clinics tend to take place in rural areas because access to health services is scarcer in these areas. Health organizations know that they can have their greatest impact in those healthcare deserts.
Mobile clinics also take place in urban areas despite the presence of more health institutions. Due to widespread poverty, individuals tend to avoid hospitals and clinics unless they are facing serious health conditions. By holding free mobile clinics, private organizations can attract people who suffer from minor illnesses. This is important because minor illnesses can often lead to more serious concerns. Ms. Pierre explains that the people who attend the clinics will complain of a backache, headache or a neck pain only to find out that they suffer from hypertension. Others who experience drastic weight loss take advantage of the glucose test and find out that they suffer from diabetes. In fact, most of the patients who attend Ms. Pierre’s mobile clinics have diabetes concerns although the organization is open to all regardless of their ailments.
For a population that lacks access to basic healthcare due to economic and/or geographic constraints, mobile clinics play an important role in preventing easily treatable diseases from developing into more serious health conditions. In the case of diabetes, Ms. Pierre claims that people who suffer from this disease will need to be educated in order to manage it well. Mobile clinics can provide this service free of charge to patients.
The Christmas day clinic
On Christmas day of 2020, Banmsantee held a mobile clinic at one of the most popular Christian churches in the city of Les Cayes. 50 people attended from 7:30 am to 1:30 pm. By the time the organization closed shop, there were no more patients to see. Most of the patients were members of the church. For that particular clinic, Banmsantee was able to gather a team of 12 volunteers that consisted of doctors, resident doctors and nurses. (See exhibit 2)
Exhibit 2. Staff for the Christmas Day Clinic
| Title | Quantity |
| Doctor | 2 |
| Resident Doctor | 6 |
| Nurse | 4 |
All in all, with 12 volunteers and 6 hours of work (36 staff hours), Banmsantee was able to tend to 50 patients; that is about 1.39 patient for every staff hour. In other words, less than 2 patients per staff hour were served during that clinic.
Planning the Mother’s Day clinic.
Banmsantee’s goal was to organize another mobile clinic after the one that took place on Christmas day. The dates of May 28, 29, 30th, 2021 were chosen to conduct the new clinic; that weekend in May coincided with Haitian Mother’s Day and the goal was to serve mostly women. Banmsantee wanted to hold the clinic on a soccer field in anticipation of greater attendance. To increase her organization’s capacity, Ms. Pierre partnered up with SOMI, a local organization involved in general prevention, HIV support and helps with orphans. This partnership meant that 25 health professionals were available for the three days of the clinic (see exhibit 3).
Exhibit 3. Staff for the Mother’s Day clinic
| Title | Quantity |
| Doctor | 2 |
| Nurses | 6 |
| Resident Nurses | 17 |
The new dates were announced in December 2020. Banmsantee purchased a megaphone and the plan was to hire a person to ride around the city and share the news of the upcoming clinic a few weeks before the event. Plans to advertise the event over the radio were also drawn up.
The Mother’s Day clinic
6 weeks before to the start of the clinic, it became clear that the event would not take place on a soccer field. The main soccer venue was hosting a game during that weekend. An alternate field was available to host for a U$ 300 fee over three days. The mobile clinics are free and not revenue generating. Banmsantee could not bear the extra cost. The organization ultimately secured 4 classrooms in a major school conveniently located in the city. Unfortunately, because school was in session on Friday, Banmsantee could only use the rooms on Saturday the 29th and Sunday the 30th (see exhibit 4).
The plan to communicate the event throughout the city did not work out either. The potential riders with the megaphone asked for too much money and that plan was no longer viable. The radio announcement could not be recorded until the location was secured. The event was starting on the 29th and the radio advertisement went out on Thursday the 27th. Attendance during the event was so low that the nurses had to recruit patients throughout the day. The event, originally designed for women, served a lot of men who were lured-in by the promise of free condoms. Ms. Pierre, despite her disappointment, believed that her team was able to save the day by getting the nurses to recruit the days of the mobile clinic. Ultimately, Banmsantee served 50 people over two days with an improvised strategy, without it the numbers could have been extremely low. For 6 hours of work per day (2 days) and 25 health care professionals (300 Staff hours), Banmsantee served 50 people; that is the equivalent of tending to 0.17 people per staff hour. In other words, Banmsantee was able to serve 1 patient per 6 staff hours (see exhibit 5).
Exhibit 4. Plan vs Actual
| Plan | Actual | |
| Staff | 25 | 25 |
| Location | Soccer field | High school |
| Advertisement | 3 months before event | 2 days before event |
| Days of service | 3 | 2 |
| Attendance expectations | More than 50 a day | About 25 per day |
Exhibit 5. Staff and performance during Christmas day vs mother’ day.
| Christmas day | Mother’s Day | |
| Staff | 12 | 25 |
| Days of service | 1 | 2 |
| Hours per day | 6 | 6 |
| Number of patients served per day | 50 | 50 |
| Patients served per staff hours | 1.39 | 0.17 |
Operations during the Mother’s Day clinic
For the Mother’s Day clinic, Banmsantee was given access to 4 classrooms that were rearranged to fit the organization’s needs (see exhibit 6).
Exhibit 6. Floor plan and Pathway
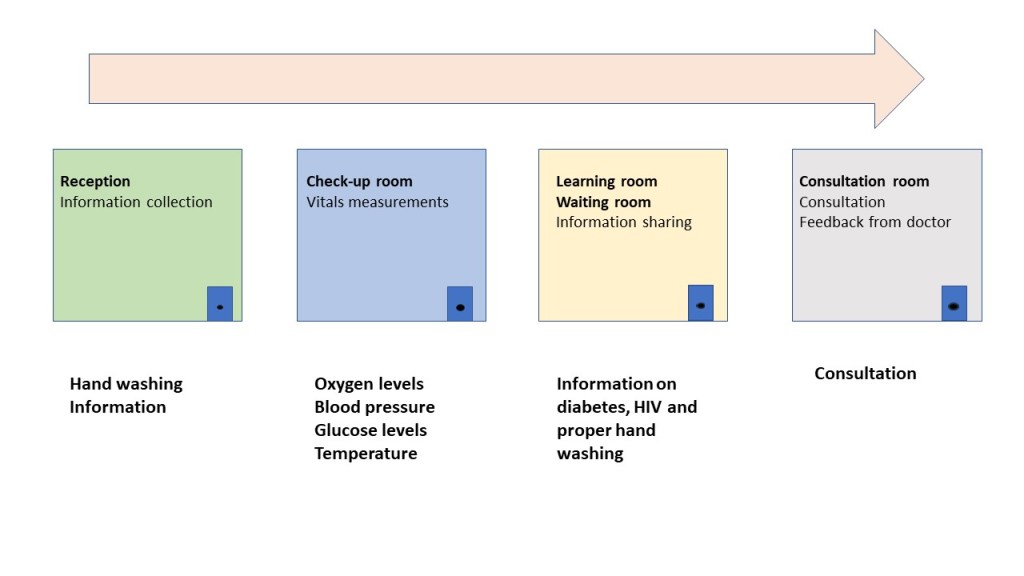
Patients are greeted by two nurses who complete the intake process. The nurses ask patients to wash their hands and respond to a series of questions to collect demographic information. The data is written down on a paper held by the patient throughout their visit. Patients move on to the check-up room where measurements for oxygen levels, blood pressure, glucose levels and temperature are taken. Patients are then directed to the next room that serves as a learning room, where they receive basic and essential information about managing diabetes, HIV and how to wash one’s hand properly. This room also serves as a waiting room until a doctor becomes available. Finally, patients proceed to a consultation room where they are screened by a doctor who gives advice and prescribes medication if need be (see exhibit 7).
Exhibit 7. The patient’s pathway and staff used
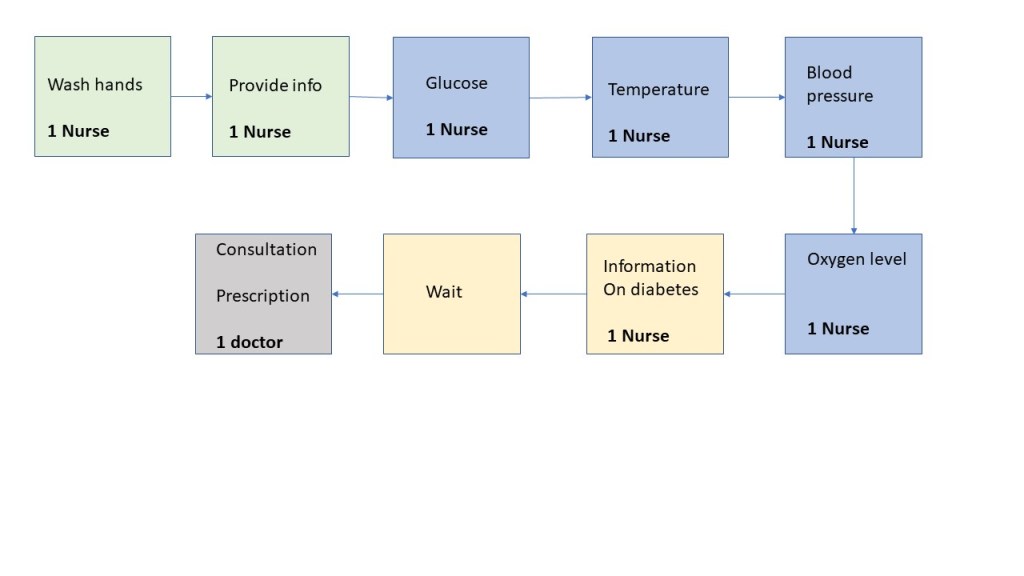
Opportunities and Challenges
The challenges that arose during the Mother’s Day mobile clinic are circumstantial and significantly impacted the original plans. Upon reflection, Ms. Pierre understands that there are opportunities for Banmsantee to improve operationally and in-turn service a greater number of patients. For example, two different nurses are not needed for hand washing and intake. One nurse could measure glucose, temperature, blood pressure and oxygen level in the same amount of time. The only reason measurements were taken by 4 different nurses was because of low attendance and the need to occupy some nurses. Banmsantee would also like to provide the information session after the consultation with the doctor if possible. The organization also provides free medical kits during these information sessions. In order to achieve that, the wait time between the check-up room and the consultation room would have to be significantly lower. Another issue is the time spent with the doctors; patients will spend between 25 to 45 minutes with the doctor. Some patients spend a lot more time talking to the doctor and Ms. Pierre believes that consultations can be kept at 30 minutes (see Exhibit 8).
Exhibit 8. Patient pathway and timeline
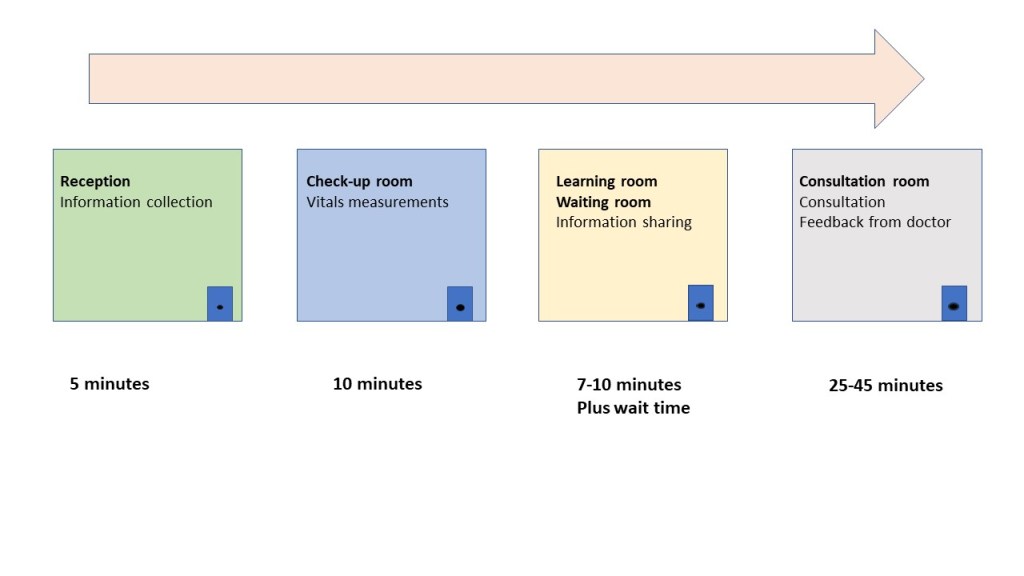
While many Haitians do not have access to medical services, there are many local doctors and nurses who remain underemployed. Ms. Pierre trusts that there is a significant opportunity to hire them occasionally for mobile clinics. So far, all the clinics have been done with local volunteers. She believes that sooner or later, Banmsantee will have to provide a stipend to incentivize involvement and sustain the mobile clinic offerings.
There are also sustainability challenges to keeping up the mobile clinics; the organization needs financial contributions in order to hold the clinics. The service may be free to patients but materials have to be paid for. In addition to buying lancets for glucose testing, the organization provides kits that carry hygienic pads, underwear and condoms. Whether volunteers get paid or not, they are provided with a hot meal, snacks, water and juice during the days they work. The organization also buys medication that is given to patients free of charge. The question of the stipend for doctors and nurses will have to come up soon or later. In the Haitian system, a doctor gets paid twice the amount of a nurse; a stipend would have to reflect that. The main operational challenge is that doctors are needed to increase the capacity of mobile clinics. The reality is that physicians cost twice as much as nurse and are more difficult to come by for volunteering opportunities.
As she sits in the airplane, Ms. Pierre tells herself that she would have to significantly ameliorate her ability to get the word out. Especially if she wants to also conduct mobile clinics in the rural areas. Are there any lessons in communication she could learn from the Christmas day clinic? She also realizes that there is no need to have many idle nurses on site, even if they are volunteers; she could gain a lot by planning her staff needs. The organization wants to significantly increase the number of patients they serve during a mobile clinic by 100%; could she redesign her operations to reach that goal without significantly increase her cost? The organization will also have to ameliorate the quality and the delivery of the service that it provides; it will need to decrease wait time so patients can go about their day. Banmsantee may have to redesign their staff requirements to achieve that. This was going to be a long flight indeed.
[1] https://www.cia.gov/the-world-factbook/countries/haiti/#people-and-society
Leave a comment